Acquired Portwine Stain on the Face in An Adult: A Case Report and Review
Received Date: May 07, 2020Accepted Date: May 16, 2020 Published Date: May 19, 2020
doi: 10.17303/croa.2020.5.103
Citation: Sreelakshmi N Nair (2020) Acquired Portwine Stain on the Face in An Adult: A Case Report and Review. Case Reports: Open Access 5: 1-4.
Abstract
Port wine stains (PWSs) also known as nevus flammeus are vascular malformations that gets its name from its appearance mimicking “port wine” (a fortified red wine) spilled on the skin. There are congenital PWSs and acquired PWSs. It can be found anywhere on the body, the most common sites being the face, neck, scalp, arms, or legs. Herein, we present a case of an acquired port-wine stain (“Fegeler syndrome) on the lower third of the face.
Keywords: port wine, acquired, lower third face
Case Report
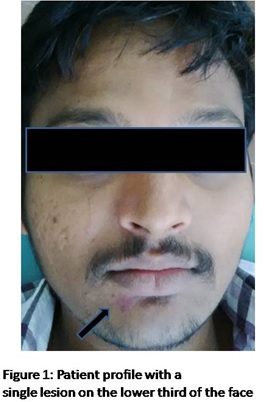
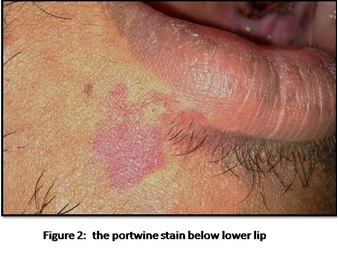
A 25 year old physically fit male patient came to our clinic for routine dental check up. Extraoral examination revealed a well defined unilateral erythematous macular lesion measuring approximately 2*3cm in size seen below the vermillion border of the lower lip on the right side (Figure 1 and 2). The area appeared non tender on palpation and slightly blanchable. There was no local rise in temperature.On anamnesis, there seemed to be no relevant history of trauma related to the erythematous area. It was believed to have appeared 4-5 years back (the patient does not clearly remember because the lesion had a slow growth but previous photographs taken during adolescent age did not show the lesion) and had been asymptomatic since then.
Taking into consideration the purpose of the patient’s visit (routine dental check up), reluctance of the patient and his family, size of the lesion (small in size and not of much cosmetic concern) and its nature (asymptomatic), a biopsy was not recommended.
Discussion
Port-wine stains are cutaneous capillary malformations, also known by the names nevus flammeus, nevus simplex or salmon patch [1]. The two types of PWS described in literature are congenital PWS which is an extensively described entity and the second type, acquired PWS which has not been reported frequently and is reported to occur post trauma to the skin even though idiopathic cases have been reported too. Morphologically both are indistinguishable from each other. Acquired PWSs were first described by Fegeler in 1949 [2]. Ours was a case of acquired PWS without a history of trauma or any other underlying causes.
Incidence
PWSs affect 0.3–1% of the population. Women tend to be affected two times more than men. In our case an adult male was affected. It is said to have a familial incidence of 10% and an autosomal dominant inheritance [3]. In our case it was acquired in later life and did not have any family history.
Etiology
The exact etiology of PWS is unknown. Few hypotheses have stated that they are formed as a result of progressive ectasia of blood vessels located in the vascular plexus of the dermis [4]. Few others suggest that acquired PWS is attributed to other causes, related to trauma, oral contraceptive pills, chronic actinic exposure, oral isotretinoin, and even cluster headache [5]. In our case, patient denied the occurrence of any prior trauma. Other etiological factors were ruled out too.
Pathogenesis
The pathogenesis of acquired PWS is not clearly understood. There have been studies suggesting malformations at the post-capillary venule and abnormalities in blood-vessel connective tissue and associated nerve supply [6].
Clinical Presentation
Both congenital and acquired PWSs clinically present with irregular borders, violaceous to-red patches and plaques.50 % of all facial PWSs happen to occur in the distribution of the trigeminal nerve[7].As age advances, color shifts from pink to purple sans changes in their size [8].Palpation of PWSs reveals that they are never warm. Our patient too had an erythematous patch but was well defined and did not show case any increase in temperature on palpation [9].
Associated syndromes
There are many known syndromes associated with congenital PWSs such as Sturge-Weber syndrome, Klippel-Trenaunay syndrome, Proteus syndrome, phakomatosis pigmentovascularis, tuberous sclerosis. But so far no syndromes have been seen associated with acquired PWSs [2]. The patient described in this case also did not showcase any of the features suggestive of any syndromes
Histological Features
Both congenital and acquired PWS have identical histologic features, characterized by ectatic capillaries and postcapillary venules lined by single endothelial cells in the papillary and superficial reticular dermis [10].
Differential diagnosis
Differential diagnosis of PWSs includes various forms of hemangiomas, tufted angiomas, Kaposi Sarcoma, and even morphea according to few studies [11].
The only entity that could be considered in our case was hemangioma which was easily ruled out as the lesion started only few years back and was not seen during the initial years after birth. As an additional diagnostic clue, hemangiomas are considered to be warm lesions whereas ours was not warm on palpation. As newer research says - diagnosis is usually made by physical examination alone and only if there are findings inconsistent with the PWSs, for example, pain or spontaneous bleeding, an MRI should be performed [12], we came to the final diagnosis of Aquired Portwine Stain on the lower third of the face.
Treatment
The Pulsed Dye Laser is most commonly used. The aim of treatment is to make the Port Wine Stain paler. Skin Camouflage, a type of special, water resistant make-up, to match up to the colour of the normal skin is considered useful too. Other treatment modalities such as embolization or skin grafting, require an extensive multi-disciplinary approach [13]. In our case, patient was not referred for any treatment as the patient was reluctant but the patient has been recalled to evaluate the progress of the lesion and to assess whether further investigations are required.
Conclusion
Most of the Acquired PWSs documented in literature have antecedent trauma as a precipitating factor even though those without trauma have also been reported. Once diagnosed, the patient can be sent for further treatment depending on the severity and extension of the lesion.
- Fegeler F (1949) Naevus flammeus in the trigeminal area after trauma as part of a post traumatic-vegetative syndrome. (Article in German). Arch Dermatol Syphilol 188: 416- 22.
- Bansal S, Garg VK, Wadhwa B, Khurana N (2015) Acquired Port-wine Stain in an Adult Male: First Reported Case from India with Review of Literature. Indian J Dermatol.60:104.
- Mitchel P. Goldman (2017) Treatment of Varicose and Telangiectatic Leg Veins. Sclerotherapy (6th edn) :81-99.
- Karvnnen SL et al. (1992) Birthmarks in 4346 Finnish newboms. Acta Derm Venereol 72:55-7.
- Pasyk KA (1993) Acquired lateral telangiectatic nevus: port-wine stain or nevus flammeus. Cutis; 51: 281–3.
- Finley JL, Clark RA, Colvin RB (1982) Immunofluorescent staining with antibodies to factor VIII, fibronectin, and collagenous basement membrane protein in normal human skin and port wine stains. Arch Dermatol. 118:971-5.
- Enjolras O, Riche MC, Meralnd JJ (1985) Facial portwine stains and sturge weber syndrome. Pediatrics.76:48-50.
- Barsky SH, Rosen S, Geer DE, Noe JM (1980) The nature and evolution of port wine stains: A computerassisted study. J Invest Dermatol 74:154–7.
- Boon LM, Vikkula M (2012) Vascular malformations. Fitzpatrick’s dermatology in general medicine. 8th edn. 2076–94.
- Thomson H (1987) Cutaneous hemangiomas and lymphangiomas. Clin Plast Surg 14:341-56.
- Pickert AJ, Carpentieri D, Price H, Hansen RC (2014) Early morphea mimicking acquired port-wine stain. Pediatr Dermatol. 31:591-4.
- Gresham TR, Adva BF (2012) Hemangiomas and vascular malformations: current theory and management. International Journal of Pediatrics Article ID 645-678.
- British association of dermatologists patient information leaflet produced august 2013 updated december 2016 review date december 2019.








Figures at a glance